We want to share some fantastic news!
On 18th January 2019, HemoGAD Technologies we were awarded a UK government research grant by Innnovate UK, part of UK Research and Innovation. The PR embargo has just been lifted by the UK government, so we can now go public.
HemoGAD Technologies Limited have been conducting research around improving the ongoing management of HH / GH. Our research project is to investigate and prove a methodology for monitoring iron levels in a home environment, with Innovate being sufficiently impressed with our concept and approach that they awarded us the maximum level of funding that is allowed under these schemes. (We still have to make a substantial financial contribution from our own resources.)
Our research is already protected under a number of (UK and International) Intellectual Property (IP) applications.
PROJECT SUMMARY – This is an extract from the project summary in our grant submission
Our Vision
This study will enable HemoGAD to accelerate the development of the world’s first rapid, discreet and non-invasive home-based Point Of Care Test (POCT) for ongoing monitoring / management, and to aid in diagnosis, of hemochromatosis severity. This has the potential to enable significant NHS cost savings and, crucially, improvements to the quality of life of hemochromatosis patients, together with other iron overload and iron deficiency sufferers.
Innovation
This test is innovative in that it will:
1) Use a saliva sample, rather than the current approach, which requires ongoing, invasive blood testing
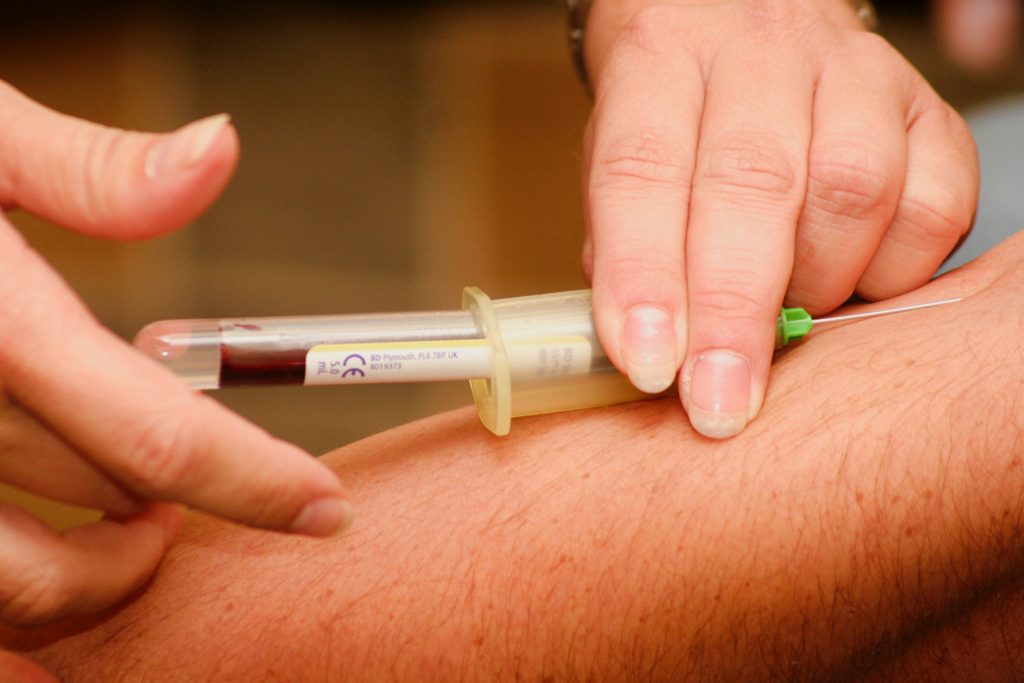
2) Be a non-invasive home use test device, rather than the current approach which requires clinician (GP, Nurse and lab) intervention and syringes
3) Provide rapid results; within 3 minutes, rather than the current approach which typically takes 1 to 3 weeks
4) Combine with a customised smartphone application (app), which uses the camera on the smartphone to take a photograph of the test result, the app then ‘calibrates’ the result to display the quantitative measurement
5) Be at a greatly reduced cost, per test, compared to the current invasive approach.
PUBLIC DESCRIPTION – this is the public description provided in our grant submission
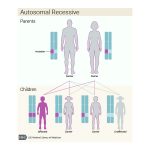
Hereditary Haemochromatosis (HH) is a genetic condition that is prevalent in people of Northern European, particularly of Celtic, descent. In Eire, Northern Ireland, Scotland and Wales – population 15 million – 1 in 80 have HH; 190,000 sufferers.
The world-wide ‘average’ is 1 in 200 people have HH. Using 1 in 200 for England (artificially low, as many English nationals have some Celtic ancestry), then UK and Eire have a minimum of 465,000 HH patients.
The World Health Organisation (WHO) state 1 in 5,000 are undiagnosed, so the number of UK sufferers is likely to be in excess of 600,000.
HH is characterised by iron overload which the body stores in the major organs. Once diagnosed, treatment is simple and effective requiring the patient to have blood taken on a regular basis – the frequency being dependent upon the severity of iron overload. Untreated, HH causes irreversible organ damage and results in chronic secondary conditions including, but not limited to:
- Cirrhosis
- Diabetes
- Heart arrhythmia
- Arthritis
- High blood pressure
HH has also been linked to Alzheimer’s (Florey Institute in Melbourne and the CSIRO), due to elevated iron levels in the brain.
Symptoms of HH include;
- Fatigue
- Joint pain
- Skin discolouration
- Loss of sex drive
- High blood pressure
This makes diagnosis difficult, as the symptoms displayed can be similar to other conditions, including anaemia. Diagnosis often comes after a patient has developed one, or more, of the totally avoidable chronic secondary conditions. This results in a negative impact on quality of life and a lifetime taking drugs to control secondary conditions – at great annual cost, per patient, to both the NHS and the patient.
Clinical diagnosis requires a specific blood test, for Serum Ferritin (SF) – a ‘general’ blood test (Full Blood Count, FBC) will not determine a patient’s iron levels. This then needs to be confirmed by genetic screening; this is expensive and time consuming for an overstretched and under-funded NHS.
HemoGAD will carry out a feasibility study around a proof-of-concept to improve diagnosis and ongoing measurement / management of iron overload, and iron deficiency. The aim is to develop a test that is:
- Faster than current methods
- Equally accurate
- Can be carried out at home
- Has a substantially lower cost
Our research project will be starting in April 2019 and should complete within 4 months. We will be providing progress updates on our BLOG and DOWNLOADS pages, where you will find regularly updated information around this exciting project.